Reduced staff over the weekends is the norm for many retail shops, but what about in healthcare?
A number of reviews have investigated the so called “weekend effect” that suggests quality of hospital care is reduced during certain periods of the week, specifically evenings and weekends. If this is true, it could result in a devastating impact for patients.
For example, as soon as an acute arterial ischaemic stroke (AIS) occurs, every second counts. It is imperative that the time taken between entering the hospital and receiving treatment, known as “door-to-needle”, is as short as possible to reduce long-term brain damage. It’s therefore important to understand if a “weekend effect” really exists. The evidence varies.
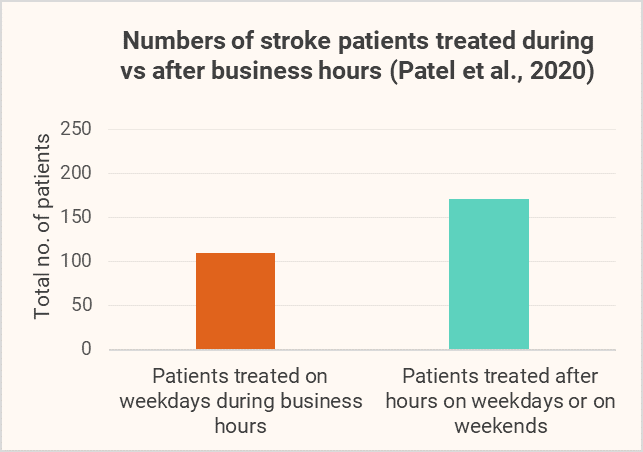
One recent study led by Dr Anand Patel from the University of Texas, retrospectively analysed data of 280 patients from their comprehensive stroke centre, publishing findings of the “weekend effect” in the journal Neurology. The study found that approximately 1/3 of the test group received treatment on weekdays during business hours, whilst the remaining 2/3 were treated after hours on weekdays or on weekends. Within the study group, treatment times were found to be significantly higher for the 61% who were treated after hours or weekends.
 However, there is contradictory evidence on the legitimacy of the “weekend effect” and stroke patient outcomes.
However, there is contradictory evidence on the legitimacy of the “weekend effect” and stroke patient outcomes.
In a separate study, assessing outcomes of stroke patients from Helsinki University Hospital, published in the Journal of Neurological Sciences, the authors stated they did not find any difference in outcome between those treated within, vs outside of normal business hours. The suggestion instead, was that with standardised procedures, an equal quality of care can be provided to patients requiring urgent treatment irrespective of time. Similarly, a Dutch retrospective study published in the Journal of Neurology looking at AIS patient outcomes, found that arriving at the hospital outside normal business hours did not lead to clinically relevant treatment delays. Within their findings, the Dutch physician reported around 60% of AIS patients were treated outside of normal business hours (defined as weekdays between 8am and 5pm). It was found that the “door-to-needle” time did increase slightly during evenings and weekends, 30 mins vs 32 mins. However, the clinical outcomes did not vary significantly between the two groups.
So, does the “weekend effect” exist and might it affect you or a loved one? The answer is: it depends.
Just as services and wait times differ between geographies, so might there be a “postcode lottery” when it comes to evening and weekend treatment outcomes. Without studying the data from a specific hospital or region, it is hard to say if they manage to maintain consistency 24/7. AIS and trauma patients are amongst those most reliant on the speed and quality of care as soon as they pass through the emergency doors. For some it may be the difference between long-term disability and recovery, and for others even life or death.
The existing treatment window for ischaemic stroke is 4.5 – 6 hours under the current guidelines. After this, a stroke patient is not eligible to receive clot-busting or removal therapies (thrombolysis or thrombectomy), as the risk of further damage to the brain outweighs the possible benefits. Tragically, estimates reveal that as few as 15% of AIS patients qualify for and receive treatment.
CLINUVEL is currently conducting a pilot clinical trial to investigate the safety and efficacy of its drug afamelanotide in AIS patients. The hope is that it will offer benefit to patients who fall outside the standard treatment window and would not otherwise receive a medical therapy. To find out more about our stroke program, click here. To understand what a stroke is and why it happens, watch our video.

Hello! Someone in my Myspace group shared this site with us so I came to look it over. I’m definitely loving the information. I’m bookmarking and will be tweeting this to my followers! Great blog and wonderful design.
I reckon something really special in this website .
I like this internet site because so much useful stuff on here : D.
Perfectly composed subject material, appreciate it for information. “The last time I saw him he was walking down Lover’s Lane holding his own hand.” by Fred Allen.
I was studying some of your articles on this internet site and I conceive this web site is very informative! Keep on posting.
whoah this blog is great i love reading your posts. Keep up the great work! You know, many people are looking around for this info, you can aid them greatly.
I am perpetually thought about this, appreciate it for putting up.
After examine a few of the weblog posts on your web site now, and I actually like your approach of blogging. I bookmarked it to my bookmark website checklist and shall be checking again soon. Pls check out my site as properly and let me know what you think.
You really make it appear so easy with your presentation but I in finding this topic to be really one thing which I feel I’d never understand. It seems too complex and very wide for me. I am taking a look ahead on your next post, I¦ll try to get the hold of it!
you have an amazing blog here! would you wish to make some invite posts on my weblog?